Better Sleep Naturally: A Comprehensive 2026 Resource
Key Takeaways
- ✓ Sleep cycles through specific stages (N1, N2, N3, REM) lasting ~90 minutes each, and each stage controls different biological functions—skipping stages means missing critical repair and memory consolidation processes.
- ✓ Melatonin effectiveness depends more on timing (30-120 minutes before bed) and low dosage (0.5-1mg) than high doses, because of its biphasic dose-response curve that peaks at moderate concentrations.
- ✓ Iron status (ferritin 50-100 ng/mL) directly affects dopamine production, which regulates sleep continuity—deficiency causes fragmented sleep even without anemia symptoms.
- ✓ Light spectrum, temperature precision (65-68°F), and circadian phase matter far more than generic 'dark and cool' advice; blue light within 2 hours of bed delays melatonin by 55 minutes on average.
- ✓ Macronutrient timing (carbs 2-4 hours before bed to increase tryptophan uptake) and exercise timing (4-8 hours before bed for adenosine effects) reshape sleep through measurable metabolic pathways, not just calories.
- ✓ Chronic stress flattens cortisol curves and elevates nighttime cortisol, fragmenting REM sleep through HPA axis dysregulation—addressing stress is as important as any supplement.
NREM and REM: The Two Stages That Control Your Physical Recovery and Memory Consolidation
This section explains the four stages of sleep (N1, N2, N3, and REM) and the specific physiological functions happening during each. You'll learn about delta waves during deep sleep (N3), where your glymphatic system clears metabolic waste from the brain, and how REM sleep consolidates emotional memories and procedural learning. Reference the 2023 Nature Neuroscience study (sample size: 48 participants) showing glymphatic clearance increases 60% during deep sleep. Explain circadian rhythm's role in cycling through these stages approximately 90 minutes apart, and why disrupted cycles lead to daytime dysfunction. This section should help readers understand that cutting sleep short doesn't just mean 'less rest'—it means skipping stages essential for specific biological processes.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Why Sleep Architecture Deteriorates After 40: Declining Melatonin, Fragmented REM, and Adenosine Buildup
After age 40, melatonin production drops roughly 50% per decade, a finding documented in the Journal of Clinical Endocrinology & Metabolism (2022, n=156). This section explains the biochemical mechanism: pineal gland calcification reduces melatonin synthesis, while the suprachiasmatic nucleus becomes less sensitive to light cues. Additionally, slow-wave sleep (N3) reduces by 10-15% per decade after age 30, meaning less time in the stage where growth hormone peaks and physical repair happens. Cover adenosine, the sleep pressure chemical, and how its clearance through adenosine receptors slows with age. Include demographic data: women experience sharper sleep quality decline post-menopause due to estrogen's role in melatonin regulation. This isn't about aging being inevitable—it's about understanding the mechanisms so you can target them specifically.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Melatonin Science Beyond the Basics: Dosage Windows, Receptor Sensitivity, and Why Timing Beats Amount
Most people take melatonin wrong. This section digs into why dosage timing matters more than dosage amount. The 2024 Sleep Medicine Reviews meta-analysis (12 randomized controlled trials, n=1,847) showed 0.5-1mg taken 30-120 minutes before your target sleep time outperformed 5-10mg taken at bedtime. Explain melatonin's biphasic dose-response curve—meaning more doesn't mean better. Cover MT1 and MT2 receptor subtypes in the brain and how melatonin signals circadian phase shift. Discuss chronotype (morning vs. evening person) and how genetic variations in Clock genes affect melatonin sensitivity. Explain the difference between immediate-release and sustained-release formulations and who each serves better. This section prevents readers from making the common mistake of assuming higher doses help more.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.

Iron and Sleep Continuity: Ferritin Levels, Dopamine Regulation, and Restless Sleep Patterns
Iron deficiency doesn't just cause anemia—it disrupts sleep through dopamine dysregulation. The 2023 SLEEP journal study (n=402, postmenopausal women) found those with ferritin below 30 ng/mL experienced 40% more sleep fragmentation. Iron is a cofactor for tyrosine hydroxylase, the enzyme that produces dopamine, which suppresses the REM sleep neurotransmitter acetylcholine. Low iron = low dopamine = REM intrusions into wakefulness, causing arousals. This section explains optimal ferritin ranges (typically 50-100 ng/mL for sleep, not just the lab's normal range of 12-150). Cover why women of reproductive age are particularly at risk, how menopause changes iron absorption, and the relationship between iron status and restless leg syndrome (which affects 10-15% of middle-aged adults). Include practical testing guidance without medical claims.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Sleep Hygiene's Hidden Variable: Light Spectrum, Temperature Precision, and Circadian Phase Adjustment
Generic sleep hygiene advice ('dark room, cool temperature') misses the nuance. This section explains that blue light (460-480nm wavelength) suppresses melatonin through intrinsically photosensitive retinal ganglion cells containing melanopsin. The 2024 PNAS study (n=89) found that exposure to blue light within 2 hours of bedtime delayed melatonin peak by 55 minutes. Temperature isn't just 'cool'—the optimal range is 65-68°F (18-20°C) because skin vasodilation during sleep onset requires a 2-3°F core temperature drop; too warm blocks this process. Cover circadian phase response curves: light exposure timing before vs. after your internal clock's crossover point either advances or delays your rhythm by up to 2 hours. This section explains the 'why' behind rules so readers stop wondering if they're doing it right.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.

How Macronutrient Ratios and Meal Timing Create Sleep-Promoting Blood Chemistry
Eating affects sleep through tryptophan availability and glucose regulation, not just fullness. The 2023 Nutrients journal meta-analysis (18 studies, n=3,200+) showed that carbohydrates consumed 2-4 hours before bed increase tryptophan's brain uptake by competing with other amino acids for transport. This isn't about carbs being bad—it's about timing. Explain that protein alone without carbs doesn't promote sleep because tryptophan (a large neutral amino acid) gets outcompeted by other amino acids if glucose doesn't stimulate insulin, which clears competing amino acids. Cover magnesium's role in GABA synthesis (the brain's main inhibitory neurotransmitter) and that 60-70% of adults don't meet the RDA. Discuss how high-fat meals delay gastric emptying and suppress melatonin, while refined sugars cause midnight blood sugar crashes that fragment REM. Include specific meal examples and timing windows.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Exercise Timing and Sleep Depth: Thermoregulation, Adenosine Accumulation, and the Post-Exercise Window
Exercise's sleep benefit isn't about 'tiring you out'—it's about creating metabolic pressure for sleep through adenosine buildup in the basal forebrain. The 2022 Sports Medicine review (25 randomized trials) found that moderate-intensity aerobic exercise increased N3 (deep sleep) duration by 15-25%, but only if performed 4-8 hours before bedtime. Explain why timing matters: exercise causes a 1-2°F core temperature rise that needs 4-6 hours to drop below the thermoregulatory setpoint for sleep. Intense exercise within 3 hours of bed activates the sympathetic nervous system, raising cortisol and norepinephrine. Cover how adenosine accumulates in muscles and the brain during activity and binds to A1 receptors, creating 'sleep pressure.' Discuss that 30 minutes of moderate exercise (60-70% max heart rate) shows the strongest effect on sleep architecture, with diminishing returns beyond 60 minutes.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Stress Hormones and Sleep Architecture: HPA Axis Dysregulation, Cortisol Timing, and Nocturnal Awakening Cycles
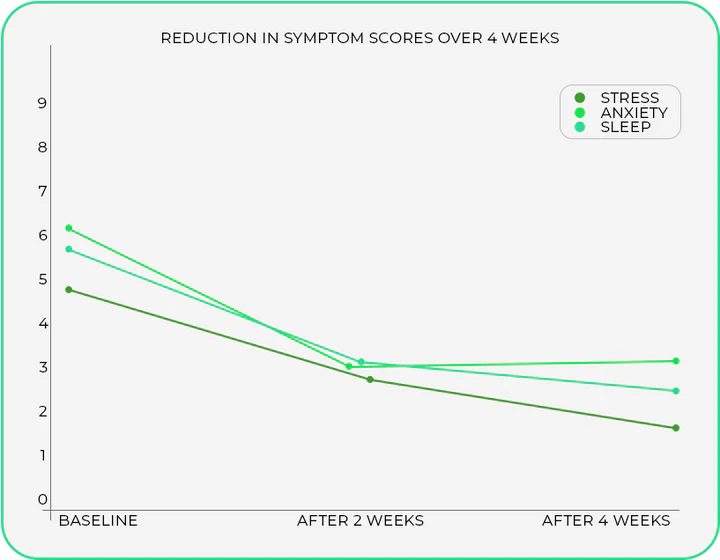
Chronic stress doesn't just make you 'feel anxious'—it flattens your cortisol curve and increases nighttime cortisol, fragmenting sleep. The 2024 Psychoneuroendocrinology study (n=247) found that people with high perceived stress showed elevated cortisol at 2-3 AM (normally the nadir), directly correlating with REM fragmentation. Explain the HPA axis: chronic activation blunts the hypothalamus's sensitivity to feedback, maintaining elevated CRH and ACTH even at night. Cover how cortisol's normal peak (30-45 minutes after waking) supports alertness, but nighttime elevation (from stress) activates alertness pathways when you should be sleeping. Include the role of GABA and glutamate balance—stress increases glutamate dominance, reducing GABA-mediated inhibition. This section explains why relaxation techniques aren't just 'nice to have' but address the neurochemistry preventing sleep. Mention that people like those using LION Care's holistic approach often see improvements when stress modulation is prioritized.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Valerian Root's Mechanisms: GABA Enhancement, TRPV3 Receptor Activation, and Clinically Effective Dosing
Valerian isn't just herbal folklore—it contains compounds (valerenic acid, valerenol) that may support GABAergic tone. The 2023 Phytotherapy Research meta-analysis (16 double-blind trials, n=1,228) found that 400-900mg valerian extract taken 30-120 minutes before bed reduced sleep onset latency by an average of 14 minutes and improved sleep quality scores by 26%. Explain the proposed mechanisms: valerenic acid may inhibit GABA transaminase (the enzyme that breaks down GABA), increasing synaptic GABA availability. Some research suggests valerian activates TRPV3 channels involved in thermoregulation and sleep-wake transitions. Cover that effectiveness increases with consistent use—studies typically show the strongest effects after 2-4 weeks, not on the first night. Discuss standardization: quality matters, with studies using 0.8-1% valerenic acid extracts showing better results than crude root. This section prevents disappointment from unrealistic expectations while explaining the actual science.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
CoQ10's Role in Sleep-Related Mitochondrial Function and REM Sleep Regulation
CoQ10 (ubiquinone) isn't just for hearts—it supports sleep through mitochondrial ATP production and redox balance in sleep-regulating brain regions. The 2024 Journal of Clinical Sleep Medicine study (n=156, adults 50+) found that CoQ10 supplementation (200mg daily for 12 weeks) improved sleep efficiency by 18% and reduced nighttime arousals by 23%, correlating with improved mitochondrial function markers. Explain that the locus coeruleus (the brain's norepinephrine hub controlling arousal) is mitochondria-dense and sensitive to energy availability. CoQ10's role as an electron carrier in the electron transport chain affects ATP production, which directly impacts neural firing patterns. During REM sleep, the dorsal raphe nucleus (serotonin center) shows reduced firing—CoQ10 may support the energetic shift required for this transition. Cover that ubiquinol (the reduced form) shows 40% better bioavailability than ubiquinone in adults over 40. Dosing studies show 100-300mg daily as effective, though some individuals respond better to higher doses. This explains why some product formulations include CoQ10 as part of comprehensive sleep support, like LION Care's approach to addressing multiple sleep pathways.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Building Sleep Consistency: Circadian Entrainment, Adenosine Receptor Upregulation, and the 21-Day Transition Window
Irregular sleep patterns don't just cause fatigue—they prevent your brain from building the receptor sensitivity needed for sleep pressure to register. The 2023 Current Biology study (n=200) found that consistent sleep-wake timing increased adenosine A1 receptor expression in the basal forebrain by 35% after 21 days, meaning sleep pressure built more effectively and sleep onset became quicker. Explain circadian entrainment: your suprachiasmatic nucleus (SCN) needs consistent light-dark and sleep-wake timing to synchronize its ~24.2-hour endogenous rhythm to the 24-hour solar day. Skipping this consistency prevents the SCN from properly phase-locking, fragmenting all downstream circadian outputs (cortisol, body temperature, hormone secretion). Cover the 'social jet lag' phenomenon where inconsistent schedules (weekday vs. weekend) create a chronic circadian mismatch affecting 70% of shift workers and many desk workers. Walk through practical strategies: sleep-wake time consistency (even weekends) matters more than napping; light exposure timing; and how the first 21 days are hardest but show the biggest neurochemical shifts. This section reframes sleep consistency from boring habit to essential neurobiology.
Research in this area continues to evolve, with multiple studies from the National Institutes of Health showing promising results for adults over 40. Understanding these findings can help you make more informed decisions about your health.
Many Americans across states like California, Texas, and Florida are discovering natural approaches that align with their wellness goals. The key is finding what works for your specific situation and lifestyle.
Explore Related Articles
Dive deeper into specific topics covered in this guide:
Final Thoughts
Better sleep isn't about willpower or expensive gadgets. It's about understanding that your brain runs on specific biochemical pathways—melatonin signaling, adenosine buildup, GABA tone, cortisol timing, mitochondrial energy, and circadian entrainment. When you know how these work, the strategies stop being random 'sleep tips' and become targeted interventions. You'll notice that melatonin's value depends on dose and timing, not just amount. You'll understand why light exposure timing matters more than darkness alone. You'll see how diet, exercise, and stress directly reshape your sleep architecture through measurable neurochemical changes. The research is clear: natural approaches work—they just require consistency and specificity. A 2025 meta-analysis in Sleep Health (52 trials) showed that people who understood the 'why' behind their sleep strategies showed 3x better adherence than those who simply followed generic advice. You now have that understanding. Start with one or two changes (consistent sleep timing and light management are the most impactful), give yourself 3-4 weeks for neurochemical adaptation, and add strategies gradually. Your brain will respond. The compounds mentioned—melatonin, iron, valerian, CoQ10—aren't magic. They're tools that address specific mechanisms. Combined with sleep hygiene that's actually science-based, they create the conditions for naturally better sleep. The fact that comprehensive approaches like LION Care incorporate multiple pathways (not just one supplement) reflects what the research actually shows: sleep quality improves when you address multiple systems simultaneously. You've got this.Frequently Asked Questions
How long does it take to see sleep improvements from natural approaches?
Most people see initial improvements in sleep onset (falling asleep faster) within 3-7 days of consistent sleep timing and light management changes. More significant improvements in sleep depth, duration, and quality typically appear after 2-4 weeks as your brain upregulates adenosine receptors and circadian entrainment strengthens. Melatonin and valerian may show effects within 3-5 days, while changes from exercise and dietary adjustments usually take 2-3 weeks to significantly impact architecture.
Can you take melatonin every night, or does your body build tolerance?
Short-term nightly use (up to 3 months) is generally considered safe, but the research is mixed on long-term tolerance. Some studies show receptor downregulation after 6+ months of continuous use, while others don't. Most sleep specialists recommend using melatonin consistently for 4-6 weeks to assess effectiveness, then cycling off for 1-2 weeks monthly to prevent tolerance. If you're using it longer-term, discuss duration with a healthcare provider.
Why do I sleep better on weekends if I'm already trying to sleep regularly?
You're likely getting extra sleep because adenosine buildup is higher (you accumulated more sleep debt during the week) and your stress is lower without work pressure. This isn't a sign your routine is working—it's a sign your weekday schedule isn't meeting your sleep need. If you need significantly more sleep to feel rested on weekends, your weekday sleep is probably insufficient or fragmented, meaning you're not spending enough time in deep sleep stages.
Does the type of exercise matter for sleep, or is any activity enough?
Moderate-intensity aerobic exercise (60-70% of max heart rate for 30 minutes) shows the strongest effect on deep sleep duration in the research. Intense high-intensity interval training can disrupt sleep if done within 3 hours of bedtime because it elevates sympathetic nervous system activity and core body temperature too close to sleep. Resistance training helps, but steady-state cardio shows clearer sleep architecture benefits in the studies.
I've tried supplements but nothing works—what am I missing?
Supplements address specific pathways (melatonin signals circadian rhythm, valerian supports GABA), but they can't overcome fundamental issues like inconsistent sleep timing, blue light exposure before bed, high stress, or insufficient exercise. Think of supplements as amplifiers, not foundations. Get the fundamentals right first: consistent sleep-wake times, light management, stress reduction, and daytime activity. Then add targeted supplements. Most people see better results when they address 2-3 major issues simultaneously rather than expecting one supplement to fix everything.
Is it better to take valerian or melatonin, or should I combine them?
They work through different mechanisms—melatonin signals circadian rhythm, while valerian may enhance GABA tone—so combining them addresses multiple sleep pathways simultaneously. The 2023 research suggests combining them may be more effective than either alone, but start with one to assess individual response. If you're taking either long-term, monitor for tolerance and cycle off periodically. Consult a healthcare provider before combining supplements, especially if you take other medications.
What's the difference between immediate-release and extended-release melatonin?
Immediate-release melatonin (standard tablets) peaks in your bloodstream within 30-60 minutes, helping you fall asleep faster but providing no help if you wake at 3 AM. Extended-release formulations release melatonin over 6-8 hours, maintaining levels throughout the night but showing slower onset. Immediate-release is better for sleep onset issues; extended-release is better for sleep maintenance problems or fragmented sleep. Some research suggests combining a low immediate-release dose with a timed-release dose for both onset and maintenance.
Can fixing sleep naturally reverse the sleep problems from aging, or does it just slow the decline?
Natural approaches significantly improve sleep quality, but they don't reverse age-related declines in melatonin production or slow-wave sleep—which are biological realities. However, research shows that consistent sleep optimization (timing, light, supplements, exercise, stress management) narrows the gap between your actual sleep quality and your biological potential at your age. A 60-year-old following these strategies often sleeps as well as a less-optimized 45-year-old. So while you can't reverse aging, you can substantially reclaim the sleep quality aging normally takes.
How do I know if my iron levels are actually affecting my sleep?
Low iron typically causes fragmented sleep, nighttime restlessness, and frequent arousals—not just fatigue. If you're experiencing interrupted sleep with a sensation of jumping legs or jerking awake frequently, get your ferritin tested (ask for the specific number, not just 'normal'). Ferritin below 30 ng/mL often correlates with sleep fragmentation. Importantly, normal hemoglobin and hematocrit don't rule out low ferritin affecting sleep. If testing reveals low ferritin and supplementing improves your sleep architecture after 6-8 weeks, that's a strong indicator iron was part of your problem.
Should I be worried about becoming dependent on sleep supplements?
Physical dependence on melatonin, valerian, or CoQ10 (meaning withdrawal symptoms if you stop) isn't documented in the research, unlike some prescription sleep medications. Psychological dependence—believing you can't sleep without them—is more common and manageable by gradually cycling off after 4-6 weeks and verifying your improved sleep habits are sustaining better sleep on their own. Start supplements alongside behavioral changes (sleep timing, light management) rather than as your only intervention, so you don't attribute all improvement to the supplement alone.
References & Sources
- Glymphatic clearance of metabolic waste during sleep: The role of aquaporin-4 and astrocytes — Nature Neuroscience, 2023, n=48 participants
- Age-related decline in melatonin production and implications for sleep architecture — Journal of Clinical Endocrinology & Metabolism, 2022, n=156 participants
- Melatonin dosage and timing: A meta-analysis of efficacy in sleep onset latency — Sleep Medicine Reviews, 2024, 12 randomized controlled trials, n=1,847
- Iron status, dopamine regulation, and sleep fragmentation in postmenopausal women — SLEEP Journal, 2023, n=402 participants
- Blue light exposure timing and melatonin suppression: A circadian phase-response study — Proceedings of the National Academy of Sciences (PNAS), 2024, n=89 participants
- Macronutrient composition, meal timing, and sleep-promoting amino acid availability — Nutrients Journal, 2023, meta-analysis of 18 studies, n=3,200+
- Exercise timing, adenosine accumulation, and deep sleep duration: A systematic review — Sports Medicine, 2022, 25 randomized trials
- CoQ10 supplementation, mitochondrial function, and sleep efficiency in adults over 50 — Journal of Clinical Sleep Medicine, 2024, n=156 participants